The undertreatment of aortic stenosis in the U.S. is severe, driven by deeply rooted racial and sex disparities and a disconnect between patients and their clinicians, according to J. Matthew Brennan, MD, MPH, an associate professor at Duke University School of Medicine who presented at TVT.19.
The problem could be fixed, but it would be hard work, said Brennan. He noted that, in the U.S., more than 65 percent of people with severe symptomatic aortic stenosis (ssAS) are untreated and that subsets of the group—including women, octogenarians and non-Hispanic blacks—are “grossly untreated.”
One factor that determines a patient's treatment path and ultimate prognosis is their cardiologist, Brennan said. Citing Optum data, he said individuals with less aggressive physicians have as much as a 20 percent increase in one-year mortality compared to their counterparts whose cardiologists are more aggressive.
“This is such a big deal that one of the biggest determinants of whether a patient actually gets treated is which cardiologist’s office they walk into,” Brennan said. “That’s as big of a determinant as their age, for example.”
Physicians also might attribute symptoms inappropriately, delay referral and treatment, inadequately inform patients of their treatment choices, misinterpret echocardiograms and miss heart murmurs, according to Brennan.
He pointed to studies suggesting both graduate medical trainees and practicing clinicians aren’t catching heart murmurs the traditional way. “We’re just not good at using our stethoscopes anymore,” he said.
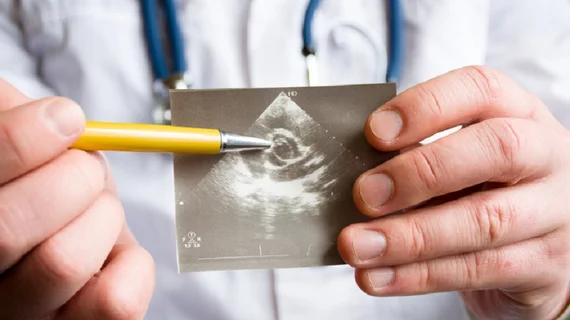
Echocardiograms are only as good as the technologists performing them and the experts interpreting them. In one study, 48 percent of severe aortic valve disease diagnoses were missed by interpreting clinicians. “That’s a problem when you’ve got a disease that progresses from mild to moderate disease to severe disease in four years,” he said. “This is not the indolent disease that we were taught about in fellowship.”
Indeed, physicians’ perception of aortic stenosis has shifted dramatically over time. The system in place to treat ssAS patients today was designed for a disease process that was only treatable with surgical interventions—a far cry from to-day’s protocol, where TAVR patients might qualify for discharge within a day of their procedure.
Moving forward, Brennan said, it will be important to address referral and treatment delays. In one study, approximately one-fourth of aortic stenosis patients waited at least five weeks from referral to treatment, which translated to an 8 percent increased risk in mortality. Another 17 percent of the patients referred for treatment never actually received it.
According to Brennan, the ideal next step would be to implement systematic follow-up of patients with aortic stenosis in each of the country’s health systems. He admitted it’s not something that happens in his own system at Duke, and he suspects the situation is similar at most centers across the U.S. “That can’t happen in today’s world,” he said. “We need to be following these patients better.”
He also suggested emphasizing objective treatment criteria over subjective symptoms, creating better tools for patient education, improving clinician training and refining technologies and techniques. “We’ve got a ways to go,” Brennan said. “This is a system that needs reforming, but our patients are worth it.”