Tectonic shifts in healthcare delivery demand a broad collective skillset measured out among cardiologists, nurses, cardiology service line directors and practice administrators. Priorities need to focus on training and outreach from clinical, operational and financial perspectives as well as strengthening the heart team. Prairie Heart and Vascular Institute in Springfield, Ill., is part of one health system that is leading the way. Working from a mission and vision combining patient care with provider education—similar to the model in place at large academic medical centers—the practice is a judicious yet eager adopter of leading-edge technologies such as Abiomed’s Impella 2.5 heart pump, the smallest and least invasive percutaneous ventricular support blood pump. Care and caregiver collaboration is a constant. In short, Prairie daily demonstrates best practices that many other heart teams would do well to emulate.
Formed in 1979 as a regional referral center in Springfield, Ill., by cardiovascular pioneer James Dove, MD, Prairie Cardiovascular Consultants Ltd. has been expanding its reach ever since. It spawned and is now part of the Prairie Heart Institute, which serves the entire southern half of Illinois from 48 locations with more than 70 board-certified cardiologists. The organization optimizes its clinical expertise and referrer outreach by sustaining a dual emphasis on ongoing skills improvement and selective technology adoption. Its hub and spoke model keeps patients in their communities and supports physicians, cardiologists and nurses. When patients need complex interventions, they head to Prairie, then optimally head back home for followup care via the Prairie web of caregivers.
It’s a model that has enabled referrer outreach to grow steadily year after year: From its humble beginnings at a single site, it has built its business to where it now logs around 180,000 unique patient visits per year.
Training, too, has been a key and ever-evolving component of Prairie’s mission. Prairie Cardiovascular runs sought-after fellowship programs not only for new and seasoned physicians from around the U.S. but also for advanced practice providers (APPs), including physician assistants as well as nurse practitioners.
A center of excellence for coronary, cardiac and vascular procedures, Prairie handles every aspect of heart care. Its expertise spans from critical limb ischemia to abdominal aortic aneurysms, from atrial septal defect and patent foramen ovale to TAVR (four per week), and from structural heart disease to high-risk PCI.
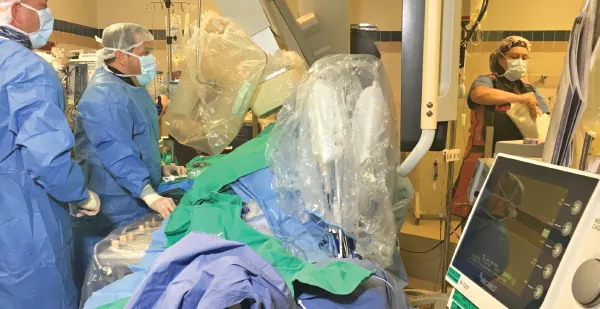
The latter exemplifies scenarios in which Prairie regularly brings all its human know-how and high-tech tools to bear on challenging clinical cases. About eight years ago, the practice became an early adopter of the first in Abiomed’s Impella line of small heart pumps. Today Prairie doctors are regularly performing Protected PCI with the recently FDA-approved Impella 2.5, saving the lives of high-risk patients who require hemodynamic support during their coronary interventions.
Supporting patients
The Impella 2.5, which can be inserted via standard catheterization through the femoral artery, stabilizes hemodynamics, unloads the left ventricle, perfuses the end organs and allows for recovery of the native heart.
“We consider the Impella an integral part of our high-risk interventional program,” says Jeffrey Goldstein, MD, who holds several leadership positions at Prairie and runs the vascular and fellowship program.
Jack Hall, MD, director of Prairie’s coronary artery chronic total occlusion (CTO) service, has much firsthand experience with Impella, as he runs the practice’s high-risk PCI program. He emphasizes the importance of selecting the right patients, knowing when to use the technology, following through with attentive care post-procedure and, perhaps most important, approaching Prairie’s work as an all-hands-on-deck endeavor.
“It’s not just about the patient and the physician inserting the Impella. It’s about your cath lab staff, it’s about the staff before the patient goes to the cath lab and it’s about the staff after the patient leaves the cath lab,” Hall says. “Educating all those people in what we’re doing and why we’re doing it” is critical. “As an interventional cardiologist, I’m only as good as the weakest person on the team and throughout that chain. At Prairie, we really focus the entire team on getting better and doing better, and that’s through education, communication and experience. We really push that hard.”
In this, he says, Abiomed has been “a huge resource for us, helping us bridge the gap” between being good, getting better and becoming the best. “They bring their clinical people in to help our nurses get familiar with [Protected PCI]. The nurses see that they don’t need to be afraid of it. We physicians are using it more often, using it earlier and getting great results, but we have to bring the rest of the staff along with us, or our results won’t be as good as they could be.”
Technology at the heart of fellowship training
Char Shallow, NP, DNP, director of Prairie’s unique fellowship program for APPs, traces Prairie’s insistence on tight teamwork to its founding. “Dr. Dove felt that it was very important that there were a number of people who were always looking after the patient to make sure they were being taken care of appropriately,” she says.
This conviction went hand-in-hand with Dove’s openness to technology, another constant at Prairie across the years. Modern device technologies such as the Impella, Shallow points out, are extending and improving life for patients who “would have never had an opportunity to live,” she says. “All of these devices are ensuring that patients are getting the care that we wouldn’t have been able to give them even five years ago.”
Specialized technology requires specialized training, which is one reason new and even experienced physicians and APPs seek out Prairie for fellowships in various aspects of cardiovascular care. The practice had for years been offering short mini-fellowships of a few days when senior physician leadership set up the Prairie Advanced Heart and Vascular Fellowship.
This 1-year “superfellowship” focuses on high-risk or complex coronary procedures, structural heart procedures and vascular procedures, as well as on caring for patients with complex heart and vascular problems. Fellows get hands-on training in these areas procedurally, and they spend time outside the lab with Prairie’s vascular internists, in the noninvasive vascular lab with its structural heart physicians and in its structural heart clinic.
Business and reimbursement matters being an ongoing concern of all healthcare professionals in these value-based-payment times, Prairie fellows get a deep dive into the ins and outs of building and maintaining a fiscally healthy cardiovascular practice. Outreach and building relationships with physicians is a priority as well.
“Even though they’re done with their interventional cardiology training, a lot of [the newer fellows] are pretty green,” says Goldstein. “It’s very gratifying to take them from day 1, where you’re constantly correcting mistakes, to day 365, when they’re operating independently and, at that point, may be better trained than me.”
Preparing APPs for the new healthcare century
Jenna Schrage, RN, BSN, MSN, is a participant in Prairie’s APP fellowship program. Educated as a family nurse practitioner, she is working her way through a 1-year fellowship in order to specialize in cardiovascular care.
“We are taught in nursing school how to correctly record what we’ve done that day in clinic so that we can get the best reimbursement possible for the services we provide,” she says when asked about the value of the business component of her Prairie APP fellowship. “Having that knowledge, along with my business knowledge from my position as outreach facilitator [for a Prairie affiliate practice], helps me understand the back end of the process, which is very different from clinical practice.
“Actually collecting the bills and getting the payments is eye-opening after being a nurse on the floor,” Schrage adds. “So going into a business role and then coming back to a clinical role, I think I’ve learned a little bit about all the aspects involved in taking care of patients.”
Shallow adds that the APP fellowship program is aimed at filling the gap APPs experience between graduation and practice. This is critical, as APPs represent the wave of the future in value-based cardiovascular health, being part indepth care monitor, part practice manager and part outreach facilitator.
“I want to bring in those nurse practitioners from out in the rural communities and give them intense training with experts,” Shallow says. “We’re going to take them from good to great, and they’re going to take those tools and bring them back to their rural communities to make sure patients have what they need to access [modern] cardiovascular care.”
Theresa Thompson, RN, BSN, client services executive who oversees Prairie Heart Institute’s clinical network development, underscores Shallow’s point and extols the virtues of a dedicated outreach arm.
“Our philosophy is to take this excellent cardiovascular care out into the community, where you start building relationships with referring physicians,” Thompson says. “They send you patients, and you take great care of their patients. You send the patients back, and the referrers send you more patients and tell other physicians about you. So your circle of friends grows. Your reputation grows.”
Not coincidentally, so does Prairie’s business, year after year.
Proactive referrer outreach, positive business results
Indeed, Prairie prides itself on its ability to build business by reinforcing existing referrer relationships while building new ones. Hall says the practice considers itself fortunate for the opportunities it has to partner with, in particular, small community hospitals throughout central and southern Illinois.
“We want to help make them great,” he says. “They’re good facilities with good people. We have the skillsets, the experience and the knowledge base, and we want to take all of that to them.”
“We want the smaller hospitals to be able to put in Impellas,” Hall adds. “Those patients may need to be transferred to us or not. As technology gets better and better, we don’t want to keep it to ourselves.”
For Goldstein, not keeping a good thing to Prairie’s own self means proactively going where the referrers are.
“We take a lot of time going to the same communities in which we see patients and giving presentations to the referring doctors, teaching them about cutting-edge therapy,” he says. “[We teach] them about the newest advances in treating structural heart disease, cardiovascular disease and so forth. So not only do we take our patient care to the communities, but we also take our knowledge to the community physicians.”
Another secret of Prairie’s business success, Thompson says, is location, location, location: Many of its outreach clinics are sited inside those small partner hospitals—and some are even inside the offices of primary care doctors. “They let us use a room or two once or twice a month or however often we go out to them,” she explains. “The expectation of the physicians who come on board for Prairie is that you will have a certain amount of windshield time. You will be going out to these communities to see patients in their communities.”
“Our overall focus is on delivering quality, data-driven care,” Goldstein says. “I hope our referring physicians know that the procedures we do are well founded in good clinical data. It’s doing what’s best for the patient. It’s contemporary, cutting-edge care for the patient that’s supported by good evidence. That’s certainly what we train our fellows in. We’re not doing a procedure just for the sake of doing a procedure. We’re doing it because it really matters for the patient.”