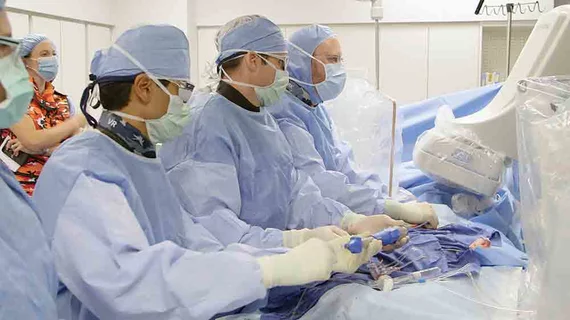
One morning last year, a patient checked into a hospital in Canada as the first transcatheter aortic valve replacement (TAVR) case of the day. That evening he checked out, an eyebrow-raising feat for a procedure that typically requires several days of hospitalization. While same-day discharge TAVR can be done, should it? For clinical and financial reasons, proceed with caution.
Pieces fell together to enable the first ever same-day TAVR discharge
François Sévigny was not your typical TAVR patient. At 65 years old, he qualified for TAVR on technical grounds. His severe aortic stenosis was considered inoperable because radiation therapy had left him with a hostile chest. He was otherwise active and functional. He had been instructed that his visit might be short, perhaps allowing him to leave the hospital by the next day. He had family to stay with him at home, which was close to the hospital.
The transfemoral procedure, the first of the day for Philippe Généreux, MD, and the rest of the heart team at Hospital of the Sacred Heart in Montreal, went without a hitch. They used conscious sedation, implanted a Sapien XT device (Edwards Lifesciences) and ascertained complete hemostasis on angiogram, all within a procedural time of 37 minutes.
When Généreux stopped by after his second TAVR case, he found the patient sitting in a chair, eating lunch. “He asked me, ‘Can I go home tonight?’ joking a little bit.” Généreux responded that if Sévigny was walking within six hours of the procedure, they could revisit the idea.
“During the third case I started thinking about this as a real possibility,” Généreux recalls. With the concurrence of the heart team, he approved the same-day discharge, requesting that Sévigny remain through dinner, just for reassurance. “I didn’t plan to do it upfront,” Généreux says. “It was purely coincidental that the patient was the first in the morning, a perfect procedure with no complication at all in a perfect patient.”
In a report on the case, Généreux and his colleagues emphasized that the patient was carefully selected and discharged after meeting numerous procedural and patient-level criteria and had no adverse events at his 30-day follow-up (Catheter Cardiovasc Interv online July 21, 2015). Reactions to the report ranged from astonishment to admonishment, he says, with some questioning the benefit over an overnight stay.
“OK, we know we can do it, but should we really do it?” he says. “The goal is to identify patients who would be able to go home safely and not come back except for their regular follow-up.”
Faster TAVR discharge and keeping patients ambulatory may be more beneficial
As TAVR devices and techniques have improved, so has an appreciation for care before and after the procedure. Besides selecting those patients most likely to benefit from TAVR, some programs strive to identify appropriate candidates for early discharge. To do so, they have expanded the concept of the heart team to include “the role of nurses, the role of geriatricians, the roles of people who understand that success is not when the valve goes in but when the patient goes home within an optimal length of stay,” says Sandra Lauck, PhD, RN, a clinical nurse specialist at St. Paul’s Hospital in Vancouver.
Lauck, and St. Paul’s colleagues David Wood, MD, and John Webb, MD, are conducting the Multidisciplinary, Multimodality but Minimalist (3M) TAVR study to evaluate the feasibility, safety and efficacy of next-day discharge using a clinical pathway to screen and manage TAVR patients. In addition to physicians’ assessment of a patient’s anatomical suitability, nurses evaluate his or her physical, mental and social function to form an individualized plan. Généreux, a 3M collaborator, consulted their discharge criteria in Sévigny’s case.
The approach tries to maximize patients’ reserve—how much gas they have in the tank going into a TAVR procedure—and minimize the stressors that can destabilize them during the admission. “We have understood that hospitals can be kind of danger zones for TAVR patients,” Lauck says. The prevailing wisdom may favor longer bed rest, but that also may put them at risk of deconditioning and other complications.
“Resting the elderly patient is not doing good,” she notes. “They need a fairly active clinical pathway to resume their baseline. The sooner they get back to baseline, the better their outcome will be.”
3M is beginning to show positive results. Danny Dvir, MD, an interventional cardiologist at St. Paul’s and a 3M researcher, reported at TCT.15 that in recent months 64 of 66 patients prospectively enrolled in 3M were discharged home safely the next day with two readmitted within 30 days. He cautions that same-day discharge remains remote, though.
“There are adverse events related to [TAVR],” Dvir says. “We should think whether the patient is at low risk of having these adverse events while he is not in the physical medical surveillance.” Those events could include conduction disturbances, a complication that is obviated in patients with a previous pacemaker, as well as stroke, bleeding and vascular complications.
Lauck and Dvir emphasize that once discharged the patient needs social support, a primary or referring physician to orchestrate continuity of care and good communication among caregivers. The overarching principles remain the same for a same-day, next-day or longer-stay discharge, Lauck says. “The bar may be higher in the same-day discharge component,” she adds. “You have to have those pieces in place. It is far more patient dependent than it is protocol dependent.”
Cost savings and penalties of early TAVR discharge
Reducing TAVR’s length of stay also can translate into cost savings for hospitals, although in the United States shorter stays also can trigger a penalty under the Post-acute Care Transfer (PACT) policy. Christopher Meduri, MD, MPH, of Piedmont Heart Institute in Atlanta, and his colleagues studied both of those scenarios in posters presented at ACC.14 and TCT.14. According to an analysis of 4,464 Medicare patients discharged after a transfemoral TAVR in 2012, the mean unadjusted length of stay was 7.7 days with a mean hospitalization cost of $61,130. Discharges at one to three days had an adjusted savings of $6,036.
“There is no doubt that reductions in length of stay will drive cost down,” Meduri says. Piedmont, which uses a minimalist approach for TAVR, has trimmed its median length of stay from six to two days between January 2014 and January 2015 for a cost reduction of $6,000 per case.
In another analysis, Meduri and Brian Potter, MD, MSc, of Beth Israel Deaconess Medical Center in Boston, assessed the impact of PACT on TAVR reimbursement and developed an app to assist discharge decision making. Lawmakers designed the policy to dissuade hospitals from discharging patients prematurely to avoid reimbursing services twice. PACT kicks in for a patient whose length of stay is less than the geometric mean (a way of measuring the mean length of stay for a diagnosis-related group nationally) with a code indicating the need for assistance within three days of discharge. That includes a skilled nursing facility, rehabilitation or home healthcare.
About 35 percent of TAVR cases in the United States triggered PACT for an average loss in reimbursement of $8,000 in 2012. “The key to that around TAVR is you have to avoid your patients needing [post-acute care],” Meduri says. “If your patients all need to go to home health or rehab and you are discharging day two or day three, your program will go broke.”
Their app helps facilities navigate this potential land mine. The app, which is free, allows a hospital to run scenarios specific to the institution’s reimbursement and patient factors to guide appropriate discharge planning. They plan to update the app with new DRG data in 2016.
While an advocate of early discharge, Meduri doesn’t see much of an upside with same-day discharge. “There will be rare exceptions of going home the same day but I think the norm should be targeting a one- or two-day length of stay instead,” he says, adding that the cost savings with same-day discharge might be $1,000 with little likelihood of filling the hospital bed after a full day’s use. “From a hospital opportunity cost, I really don’t think it will be that much of a difference.”
Généreux predicts that same-day discharge will become more commonplace with technological improvements and inclusion of intermediate-risk patients. “This would apply to a very low percentage of patients, for sure less than 5 percent,” he says. “The goal is to never compromise the safety of the patient in the name of efficiency for the system or cost savings. In 10 years it will be more feasible than now.”