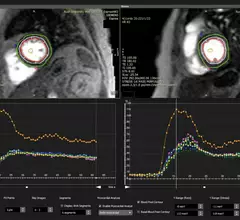
Economics
This channel highlights factors that impact hospital and healthcare economics and revenue. This includes news on healthcare policies, reimbursement, marketing, business plans, mergers and acquisitions, supply chain, salaries, staffing, and the implementation of a cost-effective environment for patients and providers.






![Pricing for coronary artery bypass grafting (CABG) varies significantly throughout the United States, according to new findings published in the Journal of the American Heart Association.[1] Researchers emphasized that higher prices were not necessarily associated with better patient outcomes. Photo by Karolina Grabowska via Pexels](/sites/default/files/styles/240x220/public/2021-08/usa_healthcare_costs.jpg.webp?itok=zB1Ej9Yo)