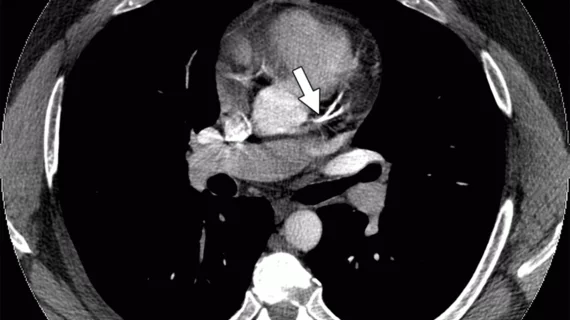
Coronary artery calcification (CAC) is often not reported in pulmonary CT angiography studies, requiring CAC assessment by radiologists in demographics at risk, according to a study published in the April issue of the American Journal of Roentgenology.
Reducing the disease burden of coronary artery disease (CAD) and managing disease progression are crucial goals in decreasing deaths due to cardiovascular disease. The study’s lead author, Connor Johnson, MD, of the Harvard Medical School in Boston, and colleagues explained: “Coronary artery calcification on chest CT is a significant predictor of cardiovascular disease events and can impact clinical care and management. CAC is associated with higher rates of arrhythmias, ischemia, hypotension, myocardial infarction, and death.”
Moreover, patients with clinical suspicion of pulmonary thromboembolism are routinely referred for pulmonary CT angiography and prediction of acute coronary syndrome (ACS) in this population is of great clinical value. Because radiologists often inconsistently record incidental findings, Johnson and colleagues evaluated the frequency at which CAC is unreported and its association with ACS in patients with pulmonary thromboembolism.
The researchers retrospectively analyzed 469 patients who were referred for pulmonary CT angiography of suspected pulmonary thromboembolism in the emergency radiology division. Results revealed that about 11.1 percent of patients had pulmonary thromboembolism and 43.8 percent had CAC. The incidence of CAC was significantly higher in patients with ACS at 56.2 percent versus those without ACS at 40.4 percent.
A strong positive association was observed between CAC and ACS in younger patients, patients without pulmonary thromboembolism and those with cardiometabolic risk factors.
CAC was not reported in 45 percent of patients with positive CAC findings on imaging. ACS was the final diagnosis in 31.6 percent of patients with unreported CAC. The data indicated a significant association between CAC and ACS in patients with unreported CAC.
“Our results showed that CAC is not reported in approximately half of patients with positive CAC findings. In our study, in the cases in which CAC was not reported, CAC was significantly associated with ACS as the final diagnosis,” wrote Johnson and colleagues. “This finding indicates that radiologists are missing a potential diagnosis for these patients.”
The study’s authors suggested further prospective studies to confirm their results. They recommended that radiologists report the presence or absence of CAC on pulmonary CT angiograms.